|
 |
|
|
 |
|
|
endometriosis Images (Click to view larger image)
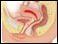
Definition
Endometriosis is caused by the presence of "endometrial like" tissue within the pelvis. This is stimulated by a woman's natural hormones resulting in bleeding and scarring within the pelvis/abdomen.
What is going on in the body?
During a woman's monthly cycle, the hormones, oestrogen and progesterone, prompt the growth of the cells that line the uterus to support a possible pregnancy. If no fertilised egg implants itself in this nourishing lining, it is shed as menstrual flow.
If cells similar to these appear outside the uterus, they respond to cyclic hormonal signals, too. However, they cannot be cast off each month. Instead, the cells cause bleeding and scars. Adhesions may weld together organs like the fallopian tubes, ovaries, or other tissues. This can cause daily or monthly cyclic pain. It may also cause infertility, if an egg cannot enter a tube or is blocked on its way down the tube to the uterus.
Endometriosis often appears in the pelvis, on the ovaries, or within the ovaries. Surfaces of the bowel, bladder, peritoneum, the membrane lining the walls of the abdomen and pelvis, and supporting ligaments may be affected. Rarely, distant areas like the lungs, liver, brain, or incision sites are affected, too.
Experts estimate the disease occurs in one in 10 women during childbearing years. It is often found among: - women who are infertile
- young teens who have severe menstrual pain or dysmenorrhoea
- women with a family history of endometriosis.
Endometriosis appears in 15% to 30% of women having a procedure called a laparoscopy. More than 50% teens with cyclic pain that does not respond to birth control pills or other medications have it, too. An unrelated condition called adenomyosis may cause similar symptoms. It is due to endometrial cells in the muscles of the uterus.
What are the signs and symptoms of the disease?
Oddly enough, some women with severe endometriosis have no symptoms. Others with very little of the disease have severe symptoms. Symptoms may include: - increasingly painful periods
- steady dull or severe pain in the lower belly during or on the days before periods
- spotty bleeding soon before periods
- painful intercourse
- pelvic pain after intercourse, pelvic examinations or exercise
- pain with bowel movements
- symptoms similar to urinary tract infections with no positive tests or cultures
- worsening menstrual cramps despite the use of birth control pills or antiprostaglandin medication
- irregular or more frequent periods
- infertility
What are the causes and risks of the disease?
No one knows just what causes this disease. There are several theories on the cause: - Endometrial cells backing up from the uterus when muscles tighten and cramp might be expelled from the fallopian tubes. Spilling into the abdominal cavity, they may implant and grow. This is the retrograde menstruation theory
- A problem with the immune system lets the cells burrow into tissue and grow in areas other than the uterine lining. This is the immune system theory.
- Some families have factors that allow for the growth of abnormal cells. This is the genetic theory.
What can be done to prevent the disease?
Experts cannot yet prevent the disease. Early diagnosis and treatment may limit cell growth and help prevent adhesions. Pregnancy, birth control pills and progesterone seems to delay the start and growth of the disease.
How is the disease diagnosed?
Right now, there are no blood tests to diagnose endometriosis. An absolute diagnosis requires surgery. Before that, a doctor may do: - A pelvic examination to find any tender nodules in ligaments that surround the uterus, tubes and ovaries. He or she also may check if pressing deeply against the uterus causes pain.
- A physical examination to find any tender nodules in scars from an episiotomy or caesarean section.
Surgical diagnosis calls for: - Laparoscopy, a tiny scope is inserted into the pelvis to help see abnormal cells and gauge the extent of the disease.
- Exploratory laparotomy, an incision in the lower belly through which a scope and tiny surgical tools may be passed. This is used for diagnosing severe disease such as adhesions, endometriomas, or hysterectomy.
What are the long-term effects of the disease?
The disease may cause no long-term serious problems. Many women are found to have had it without daily pain or infertility. When problems do occur, though, they may include: - constant pelvic pain
- pelvic or abdominal adhesions
- bowel blockage
- constant bladder or rectal pain
- infertility
- irritable bowel syndrome
- infection in the peritoneum caused by a ruptured endometrioma
- silent damage to kidneys due to uterine obstruction
What are the treatments for the disease?
Treatment is usually aimed at either managment of pain or treatment of infertility. Any treatment must consider a woman's desire to have children, her symptoms, and the extent of the disease. Age may matter, too. This disease may never be cured or eliminated. Growth can be slowed and adhesions removed to improve fertility or lessen symptoms. Options include: - Observation: Women with mild disease who are trying to get pregnant do as well with no treatment as they do with surgery or medication.
- Pain control: Antiprostaglandins, such as mefenamic acid or naproxen help control pain. They do not change the growth patterns or progress of the disease.
- Hormones: Birth control pills and high-dose progesterones may help control the disease and its symptoms.
- danazolaneme: This medication keeps the ovaries from making oestrogen in an effort to shrink errant cell growth. Danocrineis only given to women who do not want to get pregnant. It is usually taken for 6 months.
- Gonadotropin-releasing hormone (GnRH) agonists: By inhibiting the pituitary gland, these medications stop the ovary from making hormones and releasing an egg. Because bone loss is possible, GnRH agonists are only used for 6 months.
- Surgery: The goal of surgery (laparoscopy, laser, or laparotomy) is to remove endometriosis and adhesions and restore near-normal anatomy. For women with severe pelvic pain that has not responded to other techniques, cutting certain nerves in the pelvis may help. Hysterectomy and the removal of ovaries may be done if an older woman does not want children. Fertility technologies like in vitro fertilisation (IVF) have significantly improved the odds of pregnancy in women with endometriosis.
What are the side effects of the treatments?
Side effects vary depending on the treatment. Common side effects of high-dose hormones are: depression, irregular menstrual spotting or bleeding, bloating, weight gain, headaches and mood swings.
What happens after treatment for the disease?
Endometriosis recurs in 10% to 30% of cases. Despite treatment, pelvic pain may return and fertility may be impaired. The good news is that after previously infertile women have had surgery, pregnancy occurs in about: - 75% of those who had mild disease
- 50% to 60% of those who had moderate disease
- 30% to 40% of those who had severe disease
How is the disease monitored?
After treatment, worsening cramps, pelvic pain or lasting infertility may signal a recurrence. A new evaluation should be done.
Author: Eva Martin, MD
Reviewer: HealthAnswers Australia Medical Review Panel
Editor: Dr David Taylor, Chief Medical Officer HealthAnswers Australia
Last Updated: 1/10/2001
Contributors
Potential conflict of interest information for reviewers available on request |
|
 |
| |
 |
|
|
 |
 |
|
|
|