|
 |
|
|
 |
|
|
cancer of the cervix Images (Click to view larger image)
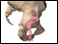
Alternative Names
cervical cancer, cervical carcinoma
Definition
The cervix is the opening between the vagina and the uterus. Cancer of the cervix is a malignant tumour on the cervix. Pre-cancerous changes in the cells on the top layer of the cervix are an early sign that cervical cancer may develop.
What is going on in the body?
Cervical cancer is fairly common cancer of the reproductive system that occurs most often among women aged 40 to 55. About 350 women in Australia die each year from cervical cancer. In fact it accounts for 4% of all cancer deaths among Australian women.
Even though the cervix is located within a woman's vagina, its cells act very much like skin cells. These cells are exposed to toxins, viruses, and bacteria that may cause abnormal changes called cervical dysplasia.
Each stage of cervical dysplasia is judged by the thickness of the layer of abnormal cells. The earliest change that can be seen with a microscope is called mild dysplasia. If not treated, these precancerous changes may become moderate and then severe. The fourth, most severe, stage of dysplasia is called carcinoma in situ. After this occurs, cancer cells may invade deeper layers of the cervix or spread to nearby sites. At that point, a woman has what is called invasive cervical cancer.
What are the signs and symptoms of the disease?
Cervical cancer that is found early usually causes no symptoms. Once the cancer invades surrounding tissues, the woman may have vague symptoms such as the following: Symptoms of more advanced cancer of the cervix include the following: What are the causes and risks of the disease?
No one knows exactly what causes cancer of the cervix. Certain health problems, lifestyle choices, and other factors may increase a woman's risk for developing it, including the following: - having had a sexually transmitted disease. Both chlamydia and human papilloma virus infections are strongly associated with cancer of the cervix.
- having had an abnormal Pap smear. A Pap smear is an examination, under a microscope, of cells scraped from the cervix.
- becoming sexually active before age 18
- having had multiple sexual partners
- not using condoms with new sexual partners
- having had cancer of the vagina or vulva
- smoking
- having a weakened immune system, for example, as a result of HIV or another immunodeficiency disorder
- being the daughter of a woman who took DES, or diethylstilbestrol, during pregnancy
- a history of cancer of the cervix in a woman's sister or mother
What can be done to prevent the disease?
Many times, cancer of the cervix can be avoided by early detection and treatment of cervical dysplasia. Cervical dysplasia can be detected by a pelvic examination that includes a Pap smear. Women should start to have Pap smears and pelvic examinations when they become sexually active.
A woman can lower her risk for getting cervical cancer by taking the following steps: - quitting smoking
- having only a few sexual partners in a lifetime
- using latex condoms and practicing safer sex with each sexual encounter
A woman should ask her sexual partners about their sexual histories, so that those who seem to be high-risk can be avoided.
Identification of early warning signs of cervical cancer is also important. A woman should see her doctor and may need to be treated if she has any of the following signs or symptoms: How is the disease diagnosed?
Diagnosis of cancer of the cervix is done with a pelvic examination that includes a Pap smear. During a pelvic examination, the cervix, vagina, and vulva are checked for signs of changes. To do a Pap smear, a doctor uses a small spatula and a brush to gently scrape cells from the cervix. These cells are sent to a laboratory for testing.
If abnormalities are found, the Pap smear may be repeated in 3 months. Alternately, the doctor may do the following additional tests: - colposcopy, a procedure in which a special microscope allows the doctor to closely examine the cervix, vagina, and vulva
- cervical biopsy, a procedure in which small tissue samples are taken from the cervix. This procedure is generally done in a doctor's office.
- cold cone biopsy, a procedure in which a large tissue sample is taken from the cervix. This procedure is normally done in an operating room under general anaesthesia. The cone biopsy often removes all of the cancerous tissue.
Tissue that is removed for a cervical biopsy is examined under a microscope and used to determine the stage of the cancer. Following are the stages of cervical cancer: - stage 1, in which the tumour is in the uterus and cervix only
- stage 2, in which the tumour has spread to the vagina
- stage 3, in which the tumour has invaded the side wall of the pelvis
- stage 4, in which the tumour has spread to the rectum, bladder, and distant organs
What are the long-term effects of the disease?
If abnormal cells are found early and treated, it may be possible to avoid removing the uterus so that a woman can still have children. Unfortunately, once cervical cancer occurs, more aggressive measures may be needed. If the cancer is found and treated early, there is an excellent chance of cure. If left untreated, it may spread to nearby areas or more distant sites in the body.
What are the risks to others?
Cervical cancer is not contagious and does not pose a risk to others. Sexually transmitted diseases associated with cervical cancer, such as chlamydia and human papilloma virus, are contagious.
What are the treatments for the disease?
If cancer of the cervix is diagnosed early, the cancer may be removed surgically. Options for surgical removal include the following: - cone biopsy, a procedure in which a portion of the centre of the cervix is removed. This procedure is also used to diagnose the cancer. During the diagnostic cold cone biopsy, the cancer is often completely removed.
- hysterectomy, or surgical removal of the uterus and cervix
If the cancer has invaded deeper layers of the cervix and has spread to the uterus, more extensive treatment may be involved, such as the following: - modified radical hysterectomy. During this type of surgery, the uterus, cervix, upper vagina, and surrounding tissue are removed. Depending on the extent of the cancer and a woman's age, the ovaries may be left in place.
- radiation therapy, which is sometimes used before or after surgery to shrink the tumour cells further
- radiation therapy and chemotherapy together. Sometimes a woman isn't a good candidate for surgery, because of her age or other medical conditions. In this instance, radiation therapy may be used alone or with chemotherapy.
- biological response modifiers, BRMs, which are substances that help to help strengthen the immune system's fight against cancer or infection. Interferon is a BRM that is sometimes used in treatment of cervical cancer, often in combination with chemotherapy.
What are the side effects of the treatments?
Possible side effects and complications of this extensive surgery are as follows: Chemotherapy and radiation therapy may cause a wide variety of side effects, including hair loss, fatigue, decreased ability to fight infections, and nausea.
Biological response modifiers such as interferon may cause flu-like symptoms, including body aches, nausea, and fatigue.
What happens after treatment for the disease?
The outcome for a woman with cervical cancer depends on many factors, such as the following: - the woman's overall health
- the woman's age when she was first diagnosed
- the type and growth of specific cancer cells
- how far the disease has spread
- the type of treatment
After treatment, the chance that a woman will live for 5 more years depends on the stage of the cancer. Survival rates for the various stages are as follows: - stage 1, 80% to 85%
- stage 2, 50% to 65%
- stage 3, 30% to 40%
- stage 4, less than 12%
How is the disease monitored?
After treatment, a woman will be closely followed for signs that the cancer of the cervix has come back. - A pelvic examination and Pap smear, if the cervix is intact, will be done every 3 months for at least 2 years and then every 6 months after that.
- Because cancer tends to come back at the same spot or spread to the lungs and liver, chest X-rays and liver function tests are done once a year.
- If a woman has had a hysterectomy, the top of the vagina is cuffed, or closed. Colposcopy may be done at follow-up visits to examine the vaginal cuff.
Any new or worsening symptoms should be reported to the doctor.
Author:
Reviewer: HealthAnswers Australia Medical Review Panel
Editor: Dr David Taylor, Chief Medical Officer HealthAnswers Australia
Last Updated: 1/10/2001
Contributors
Potential conflict of interest information for reviewers available on request |
|
 |
| |
 |
|
|
 |
 |
|
|
|