|
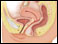
pelvic inflammatory disease Images (Click to view larger image)
Alternative Names
PID, salpingitis, salpingo-oophoritis
Definition
A woman's reproductive organs include the uterus, fallopian tubes, and vagina. Pelvic inflammatory disease or PID is an infection of these organs.
What is going on in the body?
PID can be caused by sexual intercourse or an STD. The cervix, or opening to the uterus, may allow bacteria or viruses to enter. Then, an infection may begin. This infection can spread to the fallopian tubes and other parts of the body.
What are the signs and symptoms of the disease?
There may not be any symptoms in the early stages of the disease. As the infection spreads and grows, however, the symptoms may include the following: - pain and tenderness in the lower abdomen
- heavy, foul-smelling vaginal discharge
- irregular or heavy menstrual cycles
- pain with intercourse, especially with deep penetration
- flu-like symptoms, such as fever, fatigue, backache, vomiting, or diarrhoea
- pressure in the pelvic area
- back pain that spreads down the legs
- urinary tract infection
What are the causes and risks of the disease?
A sexually transmitted disease is the most common cause of PID. The most common sexually transmitted bacteria are called Chlamydia and gonorrhoea. In some cases, bacteria that are normally found in the vagina are responsible for these infections. Sometimes the specific cause or type of bacteria cannot be found.
The disease may also occur after the pelvic organs have been manipulated in some way. This includes things such as: Childbirth puts a woman at risk for developing PID. The following conditions increase this risk: - membranes that have been ruptured for more than 24 hours before delivery
- many internal examinations during labour
- a long labour, lasting more than 12 hours
- eclampsia, also called toxaemia
- devices inserted into the uterus to monitor labour, such as foetal heart monitors
- pre-existing bacterial infection
- having a forceps delivery or caesarean section
- anaemia, or low blood count
- poor nutrition during pregnancy
- being overweight or obese
- being poor
What can be done to prevent the disease?
When a woman has procedures done in the pelvic area she is at increased risk for PID. Doctors are careful to practice sterile techniques in order to prevent an infection.
Safe sex practices help to prevent sexually transmitted diseases or STDs. This includes using condoms and either not having sex or having sex with only one person. If a woman has a sexual partner who has an STD, then she needs to be treated. If a woman thinks she has been exposed to someone with an STD, she should be treated. Some persons should consider routine checks for STDs. Such persons include sexually active teenagers, persons who have many sexual partners, and those who do not practice safe sex.
How is the disease diagnosed?
To diagnose PID a doctor reviews the woman's medical history and her symptoms. With an examination, the doctor may find the following signs: - tenderness of the uterus or lower abdomen
- tenderness or pain when the cervix is touched or moved
- discharge from the cervix
- redness and swelling of the ovaries
- tubes that have scar tissue
The doctor may want blood tests or other tests done, such as: - a full blood count, which may indicate if there is infection in the body
- sedimentation rate, a blood test that can tell if there is inflammation in the body
- bacterial or viral cultures of the cervix or vagina
- an ultrasound or a special X-ray test of the pelvic area
What are the long-term effects of the disease?
The long-term effects depend on several factors. These include the severity and length of the infection and the organisms that are causing the infection. Possible complications include: - abscess, or pocket of pus, in the tubes, ovaries, or behind the uterus
- pelvic peritonitis, an inflammation of the lining of the abdomen and pelvis
- intestinal obstruction or blockage of the bowels
- pelvic adhesions, or scar tissue in the pelvis or abdomen
- paralysed bowel
- pelvic blood clots
- destruction of the ovaries and tubes
- chronic pelvic pain syndrome
- infertility
- increased risk of ectopic pregnancy
- arthritis or swelling of the joints due to gonorrhoea infection
- skin rash
- sepsis, a serious blood infection that may lead to septic shock and death
What are the risks to others?
Because PID may be caused by a sexually transmitted disease, those with PID may transmit infections to their sexual partners.
What are the treatments for the disease?
Most women have mild to moderate symptoms. These symptoms include a fever less than 38 degrees Celsius with an abdomen that is not very tender or sore. There are no signs of shock or sepsis and the body is not reacting like it has a severe infection. Treatment in these cases includes antibiotics, analgesia, bed rest, and avoiding sexual activity. If a woman has an IUD, it will be removed.
With severe symptoms, the woman may need to be hospitalised. Higher doses of antibiotics and analgesias can be given intravenously. Fluids may be given as well. Surgery may be required.
Surgery may include draining pus through the vagina. Other procedures can include removing the injured ovaries, fallopian tubes, or any scar tissue. If the bowel is blocked, surgery can release the obstruction. A hysterectomy, or removal of the uterus, is another possible surgery.
What are the side effects of the treatments?
Side effects of antibiotics may include: Surgery may result in bleeding, worsening infection, or even death.
What happens after treatment for the disease?
Treating the infection early gives the best results. PID can cause infertility. This happens in roughly 15% of affected women. Each episode of PID increases a woman's risk of infertility. The risk of ectopic pregnancy is also increased. This is because the tubes may be blocked by scar tissue.
How is the disease monitored?
A woman may need to have more frequent cervical tests. A woman's sexual partners should also be checked and treated. Ultrasound examinations can check for an abscess that may need to be drained with surgery.
If a woman has symptoms of PID again, she should see her doctor as soon as possible.
Author: Eva Martin, MD
Reviewer: HealthAnswers Australia Medical Review Panel
Editor: Dr David Taylor, Chief Medical Officer HealthAnswers Australia
Last Updated: 1/10/2001
Contributors
Potential conflict of interest information for reviewers available on request |