|
 |
|
|
 |
|
|
type 1 diabetes mellitus Images (Click to view larger image)
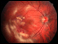
Alternative Names
insulin-dependent diabetes mellitus, Type 1 diabetes, juvenile-onset diabetes, type I diabetes
Definition
Type 1 diabetes mellitus, more commonly known as type 1 diabetes, is a disease in which the pancreas produces too little insulin to meet the body's needs. Insulin is a hormone that helps regulate the level of glucose in the blood. Glucose is the main form of sugar in the body.
What is going on in the body?
Glucose, or sugar, is an important source of energy for the cells of the body. When a person eats, the pancreas normally makes extra insulin to move glucose from the bloodstream to the inside of the cells. A person with type 1 diabetes does not have enough insulin to move glucose into the cells. The amount of glucose in the blood then becomes abnormally high, a condition called hyperglycaemia.
Type 1 diabetes is caused by an autoimmune disorder in most cases. An autoimmune disorder occurs when the body's immune system attacks the person's own body. In a person with type 1 diabetes, the pancreas, a long, thin organ located behind the stomach, is attacked by the immune system. This attack damages the pancreas so that it can no longer make enough insulin to meet the body's needs.
What are the signs and symptoms of the disease?
The symptoms of type 1 diabetes usually develop over a short period of time. Symptoms include: diabetic ketoacidosis occurs just before coma and death in people with type 1 diabetes. When the cells in the body don't get enough glucose, the body starts to burn fat for energy. This produces waste products known as ketones. High levels of ketones can result in too much acid in the body, called ketoacidosis. This condition causes dehydration, dry lips, sunken eyes, laboured breathing, vomiting, abdominal distress, and fruity-smelling breath. Immediate medical attention is needed to prevent coma and death.
What are the causes and risks of the disease?
The underlying cause of type 1 diabetes is damage to the pancreas. It's not known why this occurs in some people and not others. Genetic factors may play a factor in many cases of type 1 diabetes. It is rare in most Asian, African, and American Indian populations but more common in Caucasians. Type 1 diabetes is also more common in children and adults less than 30 years old, but it can appear at any age.
What can be done to prevent the disease?
There are at present no known ways to prevent type 1 diabetes. Although some research studies are underway.
How is the disease diagnosed?
A medical history and physical examination often lead a doctor to suspect type 1 diabetes. Diabetes is diagnosed on the basis of a high glucose level in the blood.
A blood sample can be measured at a random time or after an 8-hour fast. After an 8-hour fast, the normal blood glucose level is less than 5.5 mmols/L (millimoles per litre). A fasting blood glucose level of more than 7.0 mmols/L usually indicates diabetes.
When blood is taken randomly or without fasting first, a blood glucose level of 11.1 mmols/L or higher usually indicates diabetes.
Additional blood tests can help distinguish between type 1 diabetes and other types of diabetes. The level of ketones, for example, can be measured. Ketones are usually elevated only in type 1 diabetes.
What are the long-term effects of the disease?
Long-term effects of type 1 diabetes may include: - diabetic retinopathy, a disease in the retina of the eye that can cause blindness
- diabetic nephropathy, a disease of the kidneys that can lead to kidney failure
- arteriosclerosis, or hardening of the arteries. Arteriosclerosis can lead to heart attacks and strokes or poor circulation in the legs and feet.
- peripheral neuropathy, or damage to nerves in the limbs, which can cause numbness and pain in the hands and feet. This, along with poor circulation, can result in serious foot and leg infections that may require amputation.
- autonomic neuropathy, which may cause digestion problems, diarrhoea, erectile dysfunction in males, a rapid heartbeat, and low blood pressure
- skin infections, especially fungal infections like ringworm, and athlete's foot. Bacterial infections of the feet are also common and can be life-threatening. Amputation may be needed.
- vaginal yeast infections (thrush), because high levels of sugar encourage the growth of yeast
- urinary tract infections
- coma or death, which may occur when diabetes gets seriously out of control, usually with Diabetic ketoacidosis
What are the risks to others?
Diabetes is not contagious and poses no risk to others. Type 1 diabetes does tend to run in families.
What are the treatments for the disease?
Treatment for type 1 diabetes is focused on controlling blood glucose levels. This is done with insulin injections. Insulin can be injected under the skin a certain number of times per day, or may be given with an insulin pump. Blood glucose monitoring is done at home to help guide dose adjustments. There are many different types of insulin and the doctor can advise about what's best for each person. Insulin levels must be balanced with meals, daily activities, stress, and illness, as all of these can affect the glucose level in the blood.
Treatment also includes following a proper diet for people with diabetes and getting appropriate exercise for people with diabetes. Rarely, treatment involves receiving a transplant, which may eliminate the symptoms of type 1 diabetes. Careful monitoring and management helps keep diabetes under control and may reduce long-term effects.
Important ways for people to manage type 1 diabetes include: Treating the complications of diabetes may involve several specialists, for example, eye, heart, foot, hormone, and circulation specialists. Dieticians can help people with diabetes set up an eating plan with suggestions for kilojoule intake and types of foods to eat.
What are the side effects of the treatments?
Too much insulin in the body means blood glucose levels can drop too low. This condition is known as hypoglycaemia. It can cause nervousness, shakiness, and confusion. If this condition goes untreated, a person can pass out. The usual treatment for low blood sugar is to eat or drink something sweet. If symptoms progress to passing out, or if the person has spasms or seizures, immediate medical attention is needed.
Side effects of other treatments depend on the treatment used. A pancreas transplant is a major operation. It carries the risk of bleeding, infection, and allergic reaction to anaesthesia. To prevent rejection of the new pancreas, powerful medications with many side effects have to be taken for a long time.
What happens after treatment for the disease?
Treatment of diabetes lasts a lifetime. Type 1 diabetes cannot usually be cured, but it can be controlled with careful management and treatment. Any complications that do occur must be treated promptly.
How is the disease monitored?
Monitoring type 1 diabetes is a lifelong process. People with diabetes monitor their blood sugar daily with a finger-stick blood glucose test. There are portable devices on the market that can measure blood glucose at home. Blood tests, urine tests, foot and skin examinations, eye examinations, and visits with dieticians and other specialists are all part of routine monitoring and care for diabetes.
Author: Eileen McLaughlin, RN, BSN
Reviewer: HealthAnswers Australia Medical Review Panel
Editor: Dr David Taylor, Chief Medical Officer HealthAnswers Australia
Last Updated: 1/10/2001
Contributors
Potential conflict of interest information for reviewers available on request |
|
 |
| |
 |
|
|
 |
 |
|
|
|