|
 |
|
|
 |
|
|
prostate cancer Images (Click to view larger image)
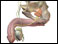
Alternative Names
adenocarcinoma of the prostate
Definition
Prostate cancer is a tumour that grows in the prostate, the gland that releases a substance that turns semen into a liquid. Normally, the prostate is a firm, walnut-shaped gland enclosed in a capsule at the base of a man's bladder. It surrounds the urethra, the tube that carries urine away from the bladder to the outside of the body.
What is going on in the body?
Prostate cancer is the most common cancer in Australian men. This type of cancer can grow slowly for many years, or it may grow rapidly and spread swiftly to other parts of the body. Another form of prostate cancer grows locally, but spreads its cells throughout the lymph system or bloodstream and along nerve sheaths.
What are the signs and symptoms of the disease?
Some men have no symptoms. Others notice common signs such as: - a need to urinate often, especially at night
- an urgent need to urinate
- dribbling when urinating
- poorer stream of urine
- blood in the urine
Prostate cancer may be detected by a digital rectal examination , or DRE, as a firm painless nodule. While it is controversial, foundations view that men should have a DRE and a blood test called a PSA about every two years from the age of 50, or as advised by their doctor. Men with a family history of prostate cancer occurring in close relatives should have the tests annually from age 40 onwards. Symptoms that the cancer has spread to other parts of the body include painful bony sites, occasional nerve paralysis, or loss of bladder function.
What are the causes and risks of the disease?
No one knows what causes prostate cancer. Hormones control the gland and may contribute to this type of cancer. It is not certain whether viruses, chronic infections, or sexual practices are also partly responsible for development of the disease. Genetics may also be a factor. So far, prostate cancer has not been linked to common cancer-causing substances in the environment.
Risk factors may include: - advanced age
- ethnic background (Prostate cancer occurs more often in African-American men than in Caucasian men, and less often in Asian men.)
- family history of cancer
- a high fat diet
Men who have had a vasectomy, use tobacco, or have been exposed to cadmium may also be at an increased risk.
What can be done to prevent the disease?
As yet, prostate cancer cannot be completely prevented. Prostate screening with examinations and blood tests help with early diagnosis, which offers the best chance for a cure. Beginning at age 50, or earlier in men with a family history of this cancer, men can have a digital rectal examination every year.
How is the disease diagnosed?
During a digital examination, a doctor puts a gloved finger into the man's rectum to feel the prostate. He or she checks for nodules or unusual firmness. Two non-cancerous conditions that cause noticeable changes in the prostate are an infection called prostatitis, and an enlargement of the prostate gland that often occurs with age, called benign prostatic hypertrophy (BPH).
The blood test for prostate specific antigen, called the PSA test, and a more refined version of it may help in diagnosing prostate cancer. High levels of PSA suggest, but cannot prove, cancer. Normal ranges for PSA increase with age.
If prostate cancer is suspected, a small sample of tissue is taken from the gland. A needle biopsy of a nodule usually gathers enough tissue. A transrectal ultrasound, which is imaging the prostate with sound waves through a probe inserted into the rectum, is needed to show the inside of the gland and any irregularities. It can be used to guide the doctor during a biopsy. Usually a number of random biopsies are also done. The tissue is sent to a laboratory where it will be checked for cancer.
Prostate cancer is graded and staged for aggressiveness and how far it has spread. - Stages A and B are cancers confined to the prostate gland.
- A stage C cancer has spread outside the gland, but only locally.
- Stage D cancer has spread to lymph nodes or distant sites in the body.
CT scans and bone scans help in staging to exclude the spread of cancer outside the prostate.
What are the long-term effects of the disease?
Long-term effects of prostate cancer depend on its stage and the type of treatment used. Some men with slow growing cancer can be monitored without treatment. Others live for a long time with prostate cancer that has spread to other sites in the body. Cancer that has spread is not curable in most cases. Unless other illnesses occur first, it usually causes death.
What are the risks to others?
Prostate cancer is not contagious.
What are the treatments for the disease?
The proper management of the many stages of prostate cancer is controversial. Depending on the grade and stage of the cancer, some options include: - watchful waiting and monitoring only
- removing part of the prostate
- removing the testes or using medications to block testosterone production
- removing the prostate and seminal vesicles
- external radiation to the prostate and pelvis
- cryosurgery to freeze cancer cells
- radioactive implants put directly into the prostate
Men with stage A and B cancers can be treated by removing the prostate and seminal vesicles, external beam radiation or radiation implants. Sometimes, a man with a stage A, B or C prostate cancer may have lymph nodes removed from the pelvis and checked to help select the best treatment. Sometimes men with a life expectancy of less than 10 years and low grade, low volume prostate cancer may choose no treatment (watchful waiting).
Hormone therapy or chemotherapy is used mostly for men with advanced stage D disease. The options include hormone therapy with anti-androgens, such as flutamide and bicalutamide, diethylstilbestrol (DES), and aminoglutethimide. Other drugs used include LHRH agonists, such as lucrin and zoladex, ketoconazole, and anti-inflammatory corticosteroids, such as prednisone.
Prostate cancer does not usually respond well to chemotherapy although newer agents such as mitozanthrone may be effective. Treatment for men with prostate cancer that has spread through the body is usually confined to making them as comfortable as possible.
A cure for prostate cancer remains controversial and continues to evolve. This is due to wide differences in the way the cancer behaves, the many acceptable treatments, and the need to minimise intervention and complications.
What are the side effects of the treatments?
People who have radiation or surgery on the prostate can still have a distant or local recurrence of the cancer. Some common side effects of these treatments are:
surgery may cause: - incontinence
- bleeding
- blood clots to leg veins and lungs
- impotence
- bowel injury (rectum)
Radiation therapy may cause: - stricture of urethra (penile tube)
- bowel inflammation and bleeding (rectum)
- bladder inflammation and poor urinary function
- impotence
- incontinence
- lethargy
Depending on exact treatment, hormonal therapy may cause: - impotence
- a higher risk of blood clots in the leg
- swelling in the breasts
- fatigue
- nausea
- bone marrow suppression
- lowered blood counts
Often given intravenously, chemotherapy has certain common side effects including: - vomiting
- lowered blood counts
- higher risk of infections
- bleeding disorders
- a higher likelihood that transfusions will be needed
Radiation implants can be painful and expensive although good results have been achieved in appropriately selected patients. These treatments may preserve sexual function. Cryosurgery should still be considered as experimental.
What happens after treatment for the disease?
After treatment, men are often monitored for side effects and a recurrence of the cancer.
How is the disease monitored?
Monitoring is done with: - digital rectal examinations
- PSA tests, which are sensitive and specific for recurrence of cancer
- ultrasound of the prostate
- CT scans of the pelvis
- chest X-rays
- bone scans
Author: Thomas Fisher, MD
Reviewer: HealthAnswers Australia Medical Review Panel
Editor: Dr David Taylor, Chief Medical Officer HealthAnswers Australia
Last Updated: 1/10/2001
Contributors
Potential conflict of interest information for reviewers available on request |
|
 |
| |
 |
|
|
 |
 |
|
|
|