|
 |
|
|
 |
|
|
diabetic foot ulcer Images (Click to view larger image)
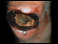
Alternative Names
diabetic foot wound, diabetic neuropathic ulceration, mal perforant ulcer, diabetic dermal ulcer, diabetic dermal wound
Definition
A diabetic foot ulcer is an open sore or wound on the foot of a person with diabetes. Because of loss of pain sensation, it is usually not painful.
What is going on in the body?
A person with diabetes often has peripheral vascular disease, or decreased circulation to the legs and feet. Any damage to the feet may heal slowly because of the poor circulation. The person may also have diabetic neuropathy, a condition in which nerve damage from diabetes causes decreased sensation in the legs and feet. The person can develop an open area from pressure or from a cut and not even feel the sore. Untreated, the damaged area can develop a diabetic foot ulcer.
What are the signs and symptoms of the condition?
Early symptoms of a diabetic foot ulcer include redness of the skin, blistering, and other signs of irritation. In later stages, the person may have an open wound that drains fluid onto socks or bedding. The open wound can then become infected and develop swelling, redness, and drainage of pus. The person may have a fever, and blood sugar levels may be higher than usual.
What are the causes and risks of the condition?
A diabetic foot ulcer is caused by direct damage to the skin, such as a cut, or by pressure, such as that from poorly fitting shoes. The following factors increase a person's chance of developing a foot ulcer: What can be done to prevent the condition?
Prevention consists of following guidelines for foot care for people with diabetes. These guidelines include regularly inspecting the feet and wearing shoes and inlays that fit properly.
How is the condition diagnosed?
Diabetic foot ulcers are usually first recognised by the affected individual. The advice of a doctor should be sought immediately. The doctor can diagnose the ulcer by looking at it. If the ulcer is draining fluid, a culture of the fluid may be sent to the laboratory to check for infection.
What are the long-term effects of the condition?
If a diabetic foot ulcer isn't treated early and effectively, a person may experience: - an infection in the ulcer itself
- septicaemia, an infection of the bloodstream, which can be caused by bacteria from the ulcer
- loss of function and ability to perform activities of daily living
- amputation of the involved foot or leg
- death
In Australia 50% of the amputations that occur in people with diabetes are preventable by good foot care and management. Most of these amputations are below the knee. After a limb has been amputated, the risk of loosing the opposite limb increases. This happens not only because of ongoing problems and vascular disease, but also because the opposite leg must bear increased pressure and workload.
What are the risks to others?
A diabetic foot ulcer is not contagious and poses no risk to others.
What are the treatments for the condition?
There are 10 major areas of treatment: - monitoring of peripheral vascular disease, which causes decreased blood flow to the feet. Monitoring includes regular measurement of oxygen levels in the skin, blood flow in the veins of the legs, and pulses in the legs and feet. In some cases, imaging with special dyes and X-rays will be used.
- monitoring of diabetic neuropathy, or nerve damage from diabetes, in the feet
- correcting risk factors. A person who smokes should quit smoking. A diet for diabetes should be carefully followed for blood sugar control. Blood pressure and cholesterol levels can be controlled with medication.
- doing regular exercise for a person with diabetes, to improve circulation to the feet. The doctor may also prescribe special support hose to improve blood flow from the legs to the heart.
- aggressively treating any sign of skin damage. The treatment may consist simply of local wound care and antibiotics. Infections, especially bone infections, must be treated surgically. It is very important to avoid pressure on the ulcer during healing because new tissue is delicate. Prescription inlays, or shoe inserts, can be used to relieve pressure on the area.
- treating any fungal infections of the foot, such as fungal nail infections, with prescription medications from the doctor
- wearing well-cushioned walking shoes, athletic shoes, or special prescription shoes as recommended by the doctor
- following a team approach to care. The team may include the person with diabetes, the primary care physician, the physician's assistant, the diabetes educator, the nutritionist, the surgical specialist and, if needed, a physician specialising in diabetes.
- performing daily foot care for a person with diabetes. In addition, the doctor should examine the person's feet at each visit.
- learning about diabetes on an ongoing basis. The individual must assume responsibility for self-care and learn how to prevent ulcers.
What are the side effects of the treatments?
All medications have side effects. For example, some of the medications used to treat diabetes may cause low blood sugar, known as hypoglycaemia, which is potentially fatal. Surgery can cause bleeding, infection, and allergic reaction to anaesthesia.
What happens after treatment for the condition?
After a person gets a diabetic foot ulcer, he or she will be at risk for further skin breakdown and infection for the rest of his or her life. Informed self-care and monitoring are the best tools available to prevent skin lesions from becoming life- and limb-threatening infections. A neglected blister or callous is the most common reason for amputations in people with diabetes.
How is the condition monitored?
A person with diabetes needs to follow foot care guidelines and monitor blood sugar levels for the rest of his or her life. Foot inspection and monitoring of diabetes, as well as any high blood pressure or high cholesterol, is also done by the doctor.
Author: Bill O'Halloran, DPM
Reviewer: HealthAnswers Australia Medical Review Panel
Editor: Dr David Taylor, Chief Medical Officer HealthAnswers Australia
Last Updated: 1/10/2001
Contributors
Potential conflict of interest information for reviewers available on request |
|
 |
| |
 |
|
|
 |
 |
|
|
|