|
 |
|
|
 |
|
|
haemorrhagic stroke Images (Click to view larger image)
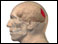
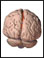
Alternative Names
stroke, brain attack, CVA, cerebrovascular accident
Definition
A stroke is the death of brain tissue that occurs when the brain does not get enough blood and oxygen. Haemorrhagic stroke is a serious condition that occurs when blood seeps into the brain tissue from a damaged blood vessel.
What is going on in the body?
A haemorrhagic stroke occurs when blood vessels in the brain burst and release blood into the area around the brain cells. The blood then damages the brain cells. The products released when cells die cause swelling in the brain. Since the skull doesn't allow much room for expansion, this swelling can damage the brain tissue even further.
What are the signs and symptoms of the condition?
Strokes can cause many different signs and symptoms, depending on the area of the brain that is damaged. Some people have multiple areas of damage. Most strokes begin suddenly, develop rapidly, and cause brain damage within minutes. Signs or symptoms may include: - problems with movement, such as weakness, clumsiness, or paralysis. These are often on only one side of the body. In some cases, people may only have weakness or clumsiness in their hand. In other cases, one entire half of the body becomes paralysed.
- headache
- numbness or a lack of feeling, which is also often on only one side of the body
- speech impairments, including slurred speech or difficulty finding the correct word
- difficulty doing math or writing
- difficulty understanding speech or writing
- inability to recognise family members or common objects
- dementia, a condition that affects memory, understanding, and the ability to carry out the normal activities of daily life
- visual impairment, including blurred vision or total vision loss
- hearing impairment
- personality changes
- difficulty swallowing
- balance problems, known as ataxia
- coma
- the inability to breathe on one's own. This may require a person to be put on an artificial breathing machine, or ventilator.
What are the causes and risks of the condition?
A haemorrhagic stroke may be caused by: - high blood pressure
- abnormal bleeding from blood-thinning medications, such as warfarin or heparin
- haemophilia A or haemophilia B, which are blood disorders that prevent normal blood clotting
- low numbers of platelets, a type of blood cell involved in blood clotting. Low platelet counts are seen in a number of diseases and conditions, including acute infections and a severe allergic reaction known as anaphylactic shock.
- rupture of a cerebral aneurysm, or weakened blood vessel wall within the brain
- sickle cell disease, an inherited condition that results in abnormal red blood cells
- a group of abnormal blood vessels within the brain known as an arteriovenous malformation or AVM
- head injuries
- eclampsia, a complication of pregnancy that causes high blood pressure in the mother
The person's risk of haemorrhagic stroke is increased if other risk factors for stroke are also present.
The risk factors for stroke can be divided into 3 categories: nonmodifiable, well-documented modifiable, and less well-documented or potentially modifiable.
The nonmodifiable factors are ones that cannot be changed by the individual and include: - increasing age. A person's risk of stroke doubles each year after age 55.
- race.
- gender. Men have a 50% higher chance of stroke than women do.
- family history of stroke or transient ischemic attack (TIA). A TIA is a short, reversible form of stroke that may serve as an early warning sign of stroke.
Well-documented modifiable risk factors are those that can be changed by the individual in conjunction with his or her doctor. These factors are linked to stroke by strong research findings, and there is documented proof that changing the risk factor lowers a person's risk of stroke. These factors include: Less well-documented or potentially modifiable risk factors for stroke are those that have less proof of either a link to stroke or the impact of modifying the risk factor. These factors include: - obesity
- a sedentary lifestyle with inadequate physical activity
- alcohol abuse
- high blood levels of homocysteine, a blood component sometimes associated with a higher risk of stroke
- drug abuse
- blood disorders, such as blood that clots easily or deficiencies of various blood components
- hormone replacement therapy (HRT). The risk of stroke associated with HRT appears low but needs further study.
- use of birth control pills, or oral contraceptives
- inflammatory processes, such as a chronic infection with chlamydia
Several recent studies have identified factors that seem to increase or decrease the risk of stroke in particular groups of people. These studies, which warrant further investigation, include these findings: - People who were treated for high blood pressure with thiazide diuretics, such as hydrochlorothiazide, had a significantly lower stroke risk than people on ACE inhibitors or calcium channel blockers.
- Women ages 15 to 44 who had 2 drinks of wine a day had a 40% to 60% lower risk of stroke than women who did not drink alcohol.
- Phenylpropanolamine, a compound contained in appetite suppressants and cold remedies, significantly increased the risk of haemorrhagic stroke in women 18 to 49 years of age.
- In one study, people who were treated in emergency departments for transient ischemic attacks (TIA) had a 25% chance of having a stroke or other serious health event within the next 90 days.
What can be done to prevent the condition?
Some haemorrhagic strokes can be prevented through careful control of the underlying disease or disorder. Careful management of sickle cell anaemia or haemophilia A or B , for example, can reduce haemorrhage strokes. For individuals with diagnosed cerebral aneurysms, guidelines for monitoring and treatment should be followed.
Haemorrhagic stroke from head injuries can be minimised by following sports safety guidelines for children, adolescents, and adults.
The prevention of stroke can be addressed with both modifiable and less well-documented or potentially modifiable risk factors.
Measures to reduce the modifiable risk of high blood pressure, a leading cause of stroke, include: - measurement of blood pressure in adults at least every 2 years to screen for high blood pressure
- weight control
- physical activity
- moderation in alcohol intake
- moderate sodium intake
- for those who smoke, quitting smoking
- medications to treat high blood pressure if the person's blood pressure is over 140/90 after 3 months of these lifestyle modifications, or if the initial blood pressure is over 180/100
Other measures to reduce an individual's modifiable risk factors for stroke may include: - smoking cessation using nicotine patches, counselling, and formal smoking programs
- control of blood sugar levels in a person with diabetes through medication, diet, and exercise
- the use of ramipril in people with diabetes. A recent study showed that people with diabetes have a 33% lower risk of stroke if they take ramipril.
- careful evaluation of asymptomatic carotid stenosis to determine the need for surgery. Coronary artery surgery, such as an endarterectomy, may be indicated. An endarterectomy opens the narrow portion of the artery and increases the blood flow to the brain. People with carotid stenosis should also work closely with their doctors to control other risk factors for stroke.
- treatment of atrial fibrillation with blood thinners such as aspirin or warfarin, depending on the person's age and other risk factors
- monitoring of high levels of total cholesterol or LDL, as well as low levels of HDL. Depending on the blood levels and the person's other risk factors, medications to lower cholesterol may be given.
Measures to reduce less well-documented or potentially modifiable risks for stroke may include: - weight reduction in overweight persons
- 30 or more minutes of moderate exercise a day for most individuals. People with heart disease or disabilities should be in a medically supervised exercise program.
- a healthy diet for heart disease, containing at least 5 fruits and vegetables a day
- for those who drink alcohol, drinking in moderation.
- seeking treatment for drug abuse
- monitoring of blood levels of homocysteine. For most individuals, a well-balanced diet following the Australian Guide To Healthy Eating will provide enough folic acid and B vitamins to maintain a healthy homocysteine level. For people with elevated homocysteine levels, supplements containing folic acid and B vitamins may be recommended.
- avoiding the use of oral contraceptives in women with other stroke risk factors
Some people have early warning signs that they are at risk for strokes. The most common warning sign is what is known as a transient ischemic attack, or TIA. This is a type of reversible stroke that often goes away after a few minutes. These people can often get treatment that will prevent a stroke in the future. For instance, people may be advised to take aspirin or have carotid artery surgery to correct a blockage in a neck artery.
How is the condition diagnosed?
Cranial MRIs and cranial CT scans may be ordered to show the type, size, and location of the stroke.
Blood tests may be done if the person is on blood-thinning medication. Blood flow tests using ultrasound or angiography may be used.
What are the long-term effects of the condition?
Strokes can cause death or permanent disability. Though many people recover some function in the first several months after a stroke, others show no improvement. Some people have several small strokes over time and slowly get worse with each one.
What are the risks to others?
Strokes are not contagious and pose no risk to others.
What are the treatments for the condition?
If someone has the early warning signs of stroke, the emergency medical system should be contacted immediately. These signs include a sudden onset of: Supportive therapy may also be needed with some strokes. This may include an artificial breathing machine, or ventilator, and an artificial feeding tube if the person cannot swallow.
Rehabilitation services can help to improve a person's function after a stroke. Physiotherapy and other therapy, such as speech therapy or occupational therapy, may be used to maximize recovery.
What are the side effects of the treatments?
Side effects depend on the treatments used. For example, a ventilator may sometimes cause damage to the lungs or an infection.
What happens after treatment for the condition?
After the person is stable, treatment of the risk factors for stroke, as well as the cause of the stroke, is important to prevent further strokes. For instance, stopping smoking and controlling high blood pressure, diabetes, and high cholesterol are advised for most people.
Many people need assistance of one form or another after a stroke. This may range from using a walking cane to needing 24-hour-a-day skilled nursing care. Ongoing therapy to improve function is usually advised for at least 6 months if the person is able.
How is the condition monitored?
People having a stroke are often admitted to the hospital for close monitoring. Once the person is stable, he or she can often be sent home or to a skilled nursing facility or rehabilitation centre for further therapy. Any new or worsening symptoms should be reported to the doctor.
Author: Gerald C. McIntosh, MD
Reviewer: HealthAnswers Australia Medical Review Panel
Editor: Dr David Taylor, Chief Medical Officer HealthAnswers Australia
Last Updated: 1/10/2001
Contributors
Potential conflict of interest information for reviewers available on request |
|
 |
| |
 |
|
|
 |
 |
|
|
|