|
 |
|
|
 |
|
|
coronary artery disease Images (Click to view larger image)

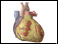
Alternative Names
coronary heart disease, arteriosclerotic coronary artery disease, ischemic heart disease, CHD, CAD
Definition
Coronary artery disease (CAD) involves the narrowing of the coronary arteries which supply blood to the heart. The arteries narrow as fatty deposits build up along the inner wall of the artery, a condition known as arteriosclerosis. Coronary artery disease is a progressive disease, which increases the risk of heart attack and sudden death.
What is going on in the body?
In order for the heart to pump normally, the heart muscle needs a continuous supply of oxygen-enriched blood. This blood is delivered by the coronary arteries. Two main vessels branch out to supply blood to the entire muscle of the heart. The heart needs more oxygen during exercise and strenuous activity. It requires less when a person is resting.
When the coronary arteries become blocked, less blood can get through. The blockage can be small or may be large enough to completely obstruct blood flow. Blockage can occur in one or many coronary arteries. Small blockages may not always affect the heart's performance.
The person may not have symptoms until the heart demands a greater amount of oxygen-rich blood than the arteries can supply. This commonly occurs during exercise or other activity. The resulting pain is called stable angina.
If a blockage is large, angina pain can occur with little or no activity, and is known as unstable angina. In this case, the flow of blood to the heart is so limited that the person cannot perform daily tasks without bringing on an angina attack. When the blood flow to an area of the heart is completely blocked, a heart attack occurs.
What are the signs and symptoms of the disease?
Symptoms of coronary artery disease vary widely and do not necessarily indicate the severity of the condition. The classic indicator of CAD is angina, or chest pain that may radiate to the neck, jaw, or left arm. The pain is often described as a crushing, burning or squeezing sensation. The person may also have shortness of breath.
Sometimes, a person may have no symptoms at all until he or she suffers a heart attack. The person may have a completely normal physical examination before the heart attack.
What are the causes and risks of the disease?
Coronary artery disease affects people of all races. It can be caused by a combination of unhealthy lifestyle and genetics. Coronary risk factors that increase the risk of CAD include: Genetic factors that affect heart disease risk are beyond a person's control. These include a strong family history of: What can be done to prevent the disease?
Although family history or genetics can't be changed, an individual can lower his or her risk for developing coronary artery disease by: How is the disease diagnosed?
A first step in diagnosing coronary artery disease is to take the person's medical history. Important factors to consider include: Also useful is an electrocardiogram, or ECG. This test may show indications of the effects of high blood pressure, areas of the heart deprived of blood, or scarring of the heart due to a previous heart attack. An ECG may be normal between attacks of angina.
Another type of test, a stress test, is basically an ECG taken before, during and after exercise. It is designed to bring on an attack of angina and record the changes that occur in the heart on an ECG. Sometimes the person is injected with a substance called thallium during the stress test. Special pictures are then taken of the heart. The thallium scan can reveal areas of the heart that are damaged.
The most reliable test for diagnosing CAD, however, remains the cardiac catheterisation. In this procedure, a thin hollow tube or catheter is inserted into an artery in the leg or arm. It is then advanced through the artery and into the coronary artery. A contrast agent is injected into the tube so the doctor can watch the blood flow through the heart and its arteries.
Other techniques that are being used to help in the diagnosis of CAD include stress echocardiograms and new generations of CT scans.
What are the long-term effects of the disease?
Coronary artery disease is a progressive disease that can lead to heart attack and sudden death.
What are the risks to others?
Coronary artery disease is not contagious, but it does tend to run in families.
What are the treatments for the disease?
Several types of medications are often used in combination to reduce the symptoms of stable angina caused by coronary artery disease. - Beta-blockers, such as atenolol or metoprolol, are used to decrease the work level of the heart, so that the same effort requires less oxygen.
- Nitrates, such as nitroglycerin or isosorbide mononitrate, help to expand the small arteries and veins. This improves the blood flow to the heart.
- Aspirin may prevent heart attacks and warfarin may prevent blood clots. However, its use in treating stable angina remains controversial.
Calcium channel blockers, such as diltiazem, nifedipine, or verapamil, have been used for over 20 years to open the coronary arteries and lower high blood pressure. However, two recent studies have found that people who take a calcium channel blocker may have a higher incidence of complications than people taking other medications for high blood pressure.
Several surgical procedures can be used to reduce the symptoms of stable angina from coronary artery disease, including: - angioplasty, a procedure in which a tube with a balloon is inserted into the blocked artery and inflated. This re-opens the artery and allows blood to flow.
- placing a stent, a rigid tube like a tiny drinking straw, into the artery at the re-opened area to keep it from narrowing again
- laser surgery, which uses light waves to dissolve plaques
- atherectomy, which involves removing plaques that cause narrowing of a blood vessel
What are the side effects of the treatments?
Side effects vary depending on the treatment used: - Beta-blockers can cause a slow heartbeat, low blood pressure, depression, erectile dysfunction, and unpleasant dreams.
- Nitrates can cause headaches and low blood pressure.
- Calcium-channel blockers can cause flushing, nausea, headache, swelling of the ankles, low blood pressure, and weakness. These medications have recently been associated with a higher risk of heart attack and congestive heart failure.
- Aspirin and warfarin increase the risk of bleeding.
- Surgery can result in infection, bleeding, allergic reaction to anaesthesia, and even death.
What happens after treatment for the disease?
Most individuals with coronary artery disease are encouraged to begin a regular exercise program. A person with CAD should make every effort to reduce coronary risk factors. This may include smoking cessation, control of other diseases such as diabetes and high blood pressure, and eating a healthy diet for heart disease. Medications may need to be adjusted to achieve the best response.
How is the disease monitored?
The person will have periodic examinations and tests by the doctor to monitor the progress of the coronary artery disease. Any new or worsening symptoms should be reported to the doctor.
Author:
Reviewer: HealthAnswers Australia Medical Review Panel
Editor: Dr David Taylor, Chief Medical Officer HealthAnswers Australia
Last Updated: 1/10/2001
Contributors
Potential conflict of interest information for reviewers available on request |
|
 |
| |
 |
|
|
 |
 |
|
|
|